10 Symptoms of Moderate or Severe Traumatic Brain Injury (TBI)
There are different medical classifications related to traumatic brain injuries (TBI); mild TBI (also known as concussion) is the most common and can develop into post-concussion syndrome if symptoms persist. However, a brain injury can also be considered moderate or severe; these types of injuries have their own set of complications. In this post, we explore these physical, cognitive and emotional symptoms associated with a more serious TBI.
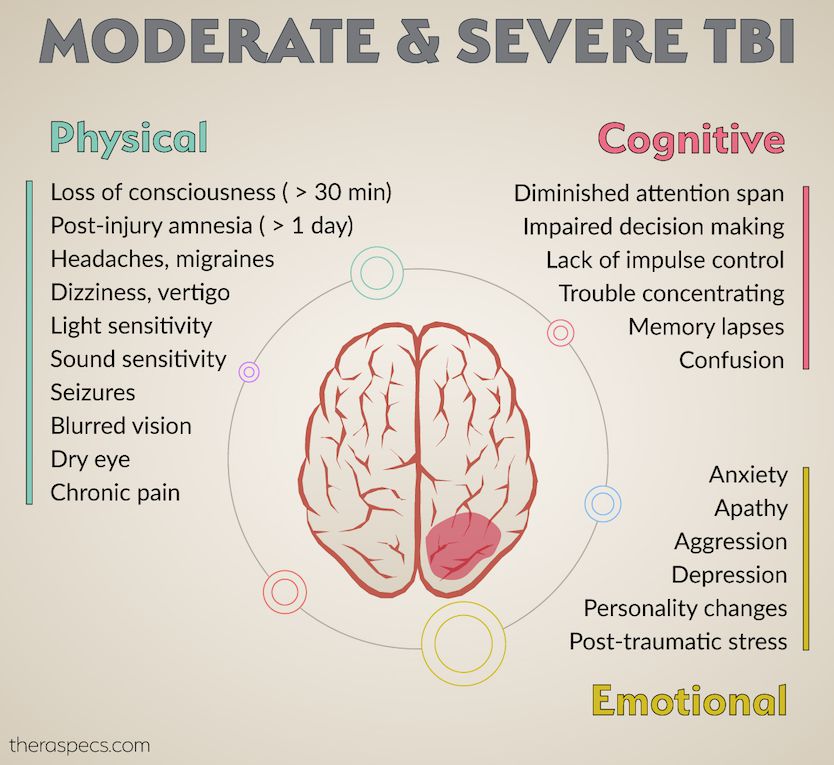
Acute symptoms of moderate or severe TBI
There are several initial signs that may indicate a possible serious brain injury. These include loss of consciousness, post-injury or post-traumatic amnesia and memory lapse, and abnormal brain imaging. Doctors grade the severity of the TBI based on the length of time that these symptoms persist.
| Acute TBI symptom | Mild | Moderate | Severe |
| Loss of consciousness | Less than 30 minutes | 30 minutes to 24 hours | Greater than 24 hours |
| Amnesia | Less than 1 day | 1 day to 7 days | Greater than 7 days |
| Brain imaging | Normal | Normal or abnormal | Normal or abnormal |
Definitions of mild, moderate and severe traumatic brain injury.1 Sourced from: https://www.ncbi.nlm.nih.gov/books/NBK299235/
Persistent moderate or severe TBI symptoms
For more critical brain injuries, patients are likely to experience a multitude of symptoms. They can manifest within a few minutes or hours of the injury or come on days or weeks later. The most common issues include (click on each below to read more):
- Headaches or migraines
- Dizziness, vertigo
- Sensitivity to light
- Sensitivity to sound
- Seizures
- Eye symptoms (dry eye, blurry vision, etc.)
- Chronic pain
- Cognitive impairment
- Disruption of sleep
- Emotional disorders
We explore each of these in depth below.
Headache and migraine
Post-traumatic headaches and migraine attacks represent some of the most common complaints after a serious head injury. Although evidence has suggested that there is no additional risk for headache-related symptoms based on severity of the TBI, between 40-50% of all TBI survivors will have these issues at various times within the first year.2 It does however increase significantly with a prior history of headache disorders. Unfortunately, even among the majority of those who make a “good” recovery, the likelihood of headache and migraine symptoms remains high.3
Dizziness, vertigo
More than half of moderate and severe brain injuries are accompanied by vertigo and/or dizziness. And how long might it last? Unfortunately, dizziness symptoms—such as lightheadedness and imbalance—may be present five years after the initial injury for as many as 37% of moderate TBI survivors and 26% of severe TBI patients. Perhaps more than any other symptom, dizziness and vertigo has been independently linked to other poor recovery and disability outcomes.4-6
Photophobia (sensitivity to light)
Photophobia, or painful light sensitivity, stemming from a serious injury to the brain has mostly been studied in military populations, but they offer some revealing insight. TBIs rated as moderate or severe can lead to light sensitivity in approximately 40% of patients; that number may be as high as 70% among those who only experience a loss of consciousness (a hallmark sign of a more serious TBI).7,8 That makes TBI-related photophobia the most common visual symptom of a critical brain injury.
Hypersensitivity to sound
Similar to light sensitivity, moderate or severe TBI can affect the perception of sound for many individuals—perhaps as many as one-quarter of patients, according to research.18 Not only can loud noises be painful for TBI survivors, but they also have a lower tolerance for noise as well.
Seizures
The type and severity of the brain injury has also been shown to increase the risk for post-traumatic seizures among TBI patients. It typically occurs less often when compared with other physical symptoms, but it can occur at just about any stage of the post-injury and recovery period. The seizure usually manifests directly in the location of the scar or contusion in the brain, leading to symptoms that include:
- Involuntary movement of specific parts of the body
- General unresponsiveness
- Inability to speak
These disturbances rarely last more than a few minutes; however, continued seizures can turn into epilepsy for TBI survivors.9,10 In addition, children are more likely to endure seizures as a result of their injury.
Eye-related symptoms
The eyes have a unique connection with the brain, and thus can be greatly affected by a serious head injury. One such concern relates to the disruption of the vestibulo-ocular reflex (VOR), which connects and stabilizes visual processing during head movements.11 Double or blurry vision also can be a problem associated with moderate or severe TBI. In addition, dry eye disease and ocular pain has also been linked to more serious TBI experiences.12
Chronic pain
Ongoing pain, regardless of location, is another feature of moderate and severe traumatic brain injuries. It can affect the neck and shoulders, the back, the head—really anywhere on the body. Studies have shown that veterans may be at even greater risk than civilians. Furthermore, depression and other emotional symptoms often increase the risk for chronic pain among TBI survivors.16
Cognitive impairment
Evidence has suggested that two out of every three survivors of severe TBI have cognitive deficits that affect their everyday mental wellbeing. These include:13
- Lapses in memory
- Diminished attention span and awareness
- Trouble concentrating
- Altered overall intelligence
- Slow or impaired decision making
- Having lack of motivation
- Displaying poor judgment
- Lack of impulse control
As a result, these concerns can dramatically impact a patient’s ongoing treatment and ability to return to normal function after the injury.
Disruption of Sleep
Studies have shown that more severe TBIs can lead to a disruption in normal sleep patterns, perhaps affecting up to 57% of individuals. This can take the form of insomnia (difficulty falling asleep) or hypersomnia (excessive sleep), with a slightly higher risk for the latter.14 Children also experience sleep disturbances, including drowsiness and impaired breathing during sleeping hours.15
Emotional disorders
Like other chronic illnesses, emotional distress is high with traumatic brain injuries. Depression, anxiety and post-traumatic stress are among the most frequent, impacting 10% to 33% of patients. Personality changes—such as apathy and aggression—also occur regularly with serious TBI. Although less common, psychosis and paranoia are known emotional complications as well.17
As noted, these are the leading symptoms of brain injuries that are classified as moderate or severe. However, these are not all the possible problems associated with serious head injuries.
At TheraSpecs, we specialize in creating precision-tinted eyewear to help light-sensitive TBI survivors find relief. If you are interested in learning how TheraSpecs might help, please click the button below.
References:
1Nelson NW, Davenport ND, Sponheim SR, et al. Blast-Related Mild Traumatic Brain Injury: Neuropsychological Evaluation and Findings. In: Kobeissy FH, editor. Brain Neurotrauma: Molecular, Neuropsychological, and Rehabilitation Aspects. Boca Raton (FL): CRC Press/Taylor & Francis; 2015. Chapter 32.
2Hoffman JM, Lucas S, Dikmen S, et al. Natural history of headache after traumatic brain injury. J Neurotrauma. 2011;28(9):1719-25.
3Rimel RW, Giordani B, Barth JT, Jane JA. Moderate head injury: completing the clinical spectrum of brain trauma. Neurosurgery. 1982 Sep;11(3):344-51.
4Berman JM, Fredrickson JM. Vertigo after head injury--a five year follow-up.J Otolaryngol. 1978 Jun;7(3):237-45.
5Maskell F, Chiarelli P, Isles R. Dizziness after traumatic brain injury: overview and measurement in the clinical setting. Brain Inj. 2006 Mar;20(3):293-305.
6Chamelian L, Feinstein A. Outcome after mild to moderate traumatic brain injury: the role of dizziness. Arch Phys Med Rehabil. 2004 Oct;85(10):1662-6.
7Bulson R, Jun W, Hayes J. Visual symptomatology and referral patterns for Operation Iraqi Freedom and Operation Enduring Freedom veterans with traumatic brain injury. J Rehabil Res Dev. 2012;49(7):1075-82.
8Goodrich GL, Flyg HM, Kirby JE, Chang CY, Martinsen GL. Mechanisms of TBI and visual consequences in military and veteran populations. Optometry and vision science : official publication of the American Academy of Optometry. 2013 Feb;90(2):105–112.
9Englander J, Bushnik T, Duong TT, et al. Analyzing risk factors for late posttraumatic seizures: a prospective, mulitcenter investigation. Arch Phys Med Rehabil. 2003;84:365–373.
10Englander J, Cifu DX, Diaz-Arrastia R. Information/education page. Seizures and traumatic brain injury. Arch Phys Med Rehabil. 2014;95(6):1223-4.
11Wallace B, Lifshitz J. Traumatic brain injury and vestibulo-ocular function: current challenges and future prospects. Eye Brain. 2016;8:153-164. Published 2016 Sep 6. doi:10.2147/EB.S82670.
12Lee CJ, Felix ER, Levitt RC, et al. Traumatic brain injury, dry eye and comorbid pain diagnoses in US veterans. British Journal of Ophthalmology Published Online First: 26 August 2017. doi: 10.1136/bjophthalmol-2017-310509.
13Rabinowitz AR, Levin HS. Cognitive sequelae of traumatic brain injury. Psychiatr Clin North Am. 2014;37(1):1-11.
14Hou L, Han X, Sheng P, et al. Risk factors associated with sleep disturbance following traumatic brain injury: clinical findings and questionnaire based study. PLoS One. 2013;8(10):e76087. Published 2013 Oct 1. doi:10.1371/journal.pone.0076087.
15Bogdanov S, Brookes N, Epps A, Naismith SL, Teng A, Lah S. Sleep Disturbance in Children With Moderate or Severe Traumatic Brain Injury Compared With Children With Orthopedic Injury. J Head Trauma Rehabil. 2018 Jul 24. doi: 10.1097/HTR.0000000000000426. [Epub ahead of print]
16Seal KH, Bertenthal D, Barnes DE, Byers AL, Strigo I, Yaffe K. Association of Traumatic Brain Injury With Chronic Pain in Iraq and Afghanistan Veterans: Effect of Comorbid Mental Health Conditions. Chronic Effects of Neurotrauma Consortium Study Group. Arch Phys Med Rehabil. 2017 Aug;98(8):1636-1645. doi: 10.1016/j.apmr.2017.03.026. Epub 2017 Apr 25.
17Schwarzbold M, Diaz A, Martins ET, et al. Psychiatric disorders and traumatic brain injury. Neuropsychiatr Dis Treat. 2008;4(4):797-816.
18Dikmen S, Machamer J, Fann JR, Temkin NR. Rates of symptom reporting following traumatic brain injury. J Int Neuropsychol Soc. 2010 May;16(3):401-11. doi: 10.1017/S1355617710000196. Epub 2010 Mar 1.

TheraSpecs® Glasses for Light Sensitivity
Find the glasses that fit your needs and lifestyle, and stay protected from screens, fluorescents, unwanted blue light, sunlight, flashing lights, and more.
Shop Now



