7 Alternatives for Natural Migraine Relief, Prevention, and Management
If you live with migraine, it’s likely you are aware that specific triggers and treatments vary from person to person, making consistent migraine relief a moving target. Moreover, migraine drugs can complicate things with ineffective results, compounding side effects and concerns of medication overuse headache. However, there are several alternative treatments that can provide natural migraine relief and prevention without the need for prescription medication. Although each patient experience can be different, these remedies are generally supported by clinical research and are frequently recommended by headache specialists and neurologists. But what do you know about the effectiveness and cost of these solutions? We break down everything you should know about these alternative migraine treatments.
Note: ALWAYS consult with your doctor before trying any treatment strategies. Your doctor can help you determine which remedies are best for you, and it is essential to discuss any option with them to ensure it is safe and appropriate.
1. Acupuncture
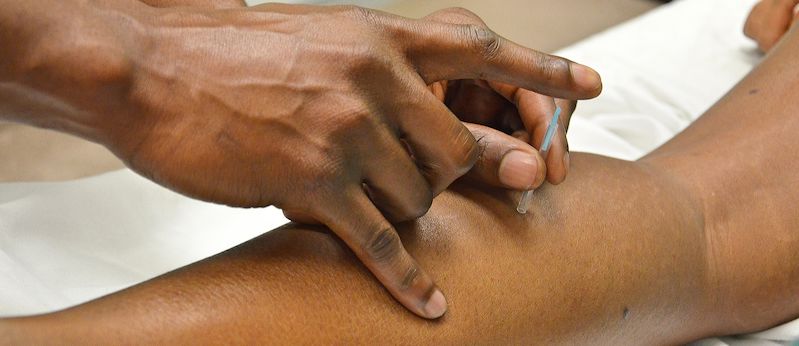
Acupuncture has been used as an option for migraine prevention for many years. Specialists in this field insert very fine needles into specific points on the body, then manually or electrically stimulate the needles. The practice promotes blood flow into the areas around the needles, which may help with migraines.
Research and effectiveness
Research has been mixed about the effectiveness of acupuncture, but there have been several studies highlighting a reduction in the number of migraine attacks and intensity of those attacks, even after 12 weeks.1 Another study showed that the number of headache days were nearly cut in half when compared with those who did not have acupuncture; pain intensity and quality of life were also improved and persisted for up to 6 months.2 Although there has been a high potential for placebo-related benefits—as evidenced by comparable results for “sham” acupuncture treatments—it has been recommended by the American Headache Society and other experts based on the premise that it is at least as reliable as other migraine prevention strategies.
Side effects
Acupuncture is generally regarded as a safe alternative treatment for migraines. However, there are some occasional side effects that have been reported by approximately 10% of individuals.3 These may include:
- bruising
- soreness
- bleeding at the needle site
- feelings of heaviness
- numbness
- tingling.
Cost
One of the bigger drawbacks of acupuncture relates to the cost. Advocates from migraine.com have estimated the cost of acupuncture for migraine at $50 to $120 per session. Coupled with the need for multiple sessions per week (to be effective) as well as the inconsistency in insurance coverage, and the out-of-pocket expense could number in the thousands. This is supported by further research that costs to patients utilizing acupuncture are higher during the treatment period; however, they also have observed longer-term reduction in migraine-related costs after one year due to the positive benefits reported by many patients.4
2. Biofeedback

Biofeedback has been an accepted option for relief for migraines for some time. In effect, it teaches patients to control involuntary bodily processes like heart rate and muscle tension by utilizing electronic monitoring. By bringing awareness to these physiological changes, doctors and other professionals can help them develop techniques to manage any negative effects.
Research and effectiveness
Like acupuncture, the National Headache Foundation and American Headache Society both acknowledge the validity of biofeedback as an effective tool for migraine patients. They are basing these recommendations on studies that have shown 7 out of 10 individuals have experienced a 70% reduction in migraine attacks—results that continued for more than a year.5 Although biofeedback also did not yield enough significant difference compared with placebo treatments or other relaxation techniques, there was enough positive benefit when compared with the control groups who were not being treated with biofeedback.6-7 Many prominent advocacy organizations suggest that biofeedback is most effective when combined with other therapies for treating migraine.
Side effects
Biofeedback, conducted with the guidance of a trained professional is safe and free of side effects. However, if improperly applied, can result in an exacerbation of symptoms.8
Cost
Although the long-term benefits of biofeedback may validate its use, the cost can be high, which has been listed at somewhere between $35 to $85 per treatment. Some researchers have argued biofeedback is not a cost-effective alternative for migraine prevention due to the number of sessions required—which might be 10 or more—thus bring the direct cost to hundreds, maybe even thousands of dollars. However, some migraineurs have noted that health insurance may be able to assist with the cost.
3. Precision-tinted FL-41 lenses

For those with migraine-related light sensitivity or light triggers, TheraSpecs precision-tinted FL-41 lenses are a great option to naturally provide relief and prevent migraine attacks from happening...all without having to deal with prescribed medication. This tint removes very specific wavelengths of blue light that aggravate or trigger pain responses for people with migraine.9 This gives the lenses a rose color and can be worn regularly around common light sources such as fluorescent light, computer or mobile device screens, and sunlight.
Research and effectiveness
There have been a few primary studies supporting the value of precision tinted lenses for migraine. The first showed that children who used glasses with this tint experienced 74% fewer attacks, and the benefits lasted for at least four months.10 Other studies have shown that the tint can reduce sensitivity to and flicker in fluorescent lighting as well as overall sensitivity to light and pain.11 In our experience, nine out of ten TheraSpecs customers report some level of relief for their migraine attacks and light sensitivity, providing anecdotal support for the research. There has been additional evidence for the use of precision tinted glasses for other light-sensitive conditions such as blepharospasm, concussion and photosensitive epilepsy; however, these studies have not validated the specific tint explored in prior research.12-14 There are also other colored lenses that claim to help people with migraine, but only the TheraSpecs tint has been meaningfully studied. Read our analysis of these other tints.
Side effects
There have been no clinical findings showing any side effects of tinted lenses. Some patients have questioned whether there is a dependence-like effect after wearing these glasses for an extended period of time—such that taking them off results in worsened light sensitivity. However, there is no evidence that this is the case; in fact, wearing dark sunglasses indoors is the only behavior that is shown to result in more pronounced sensitivity to light, according to migraine experts.
Cost
Unlike other treatments that require repeated sessions and a significant time commitment, precision tinted lenses like TheraSpecs are a one-time purchase. For example, TheraSpecs glasses (non prescription) typically range from $99 to $278 and are guaranteed by a 60-day return policy. It’s important to remember that FL 41 lenses are not likely to reduce all migraine attacks, but can make a significant impact on light-triggered episodes.
4. Relaxation, meditation, and stress management

Relaxation and meditation techniques show promise for people with chronic migraine, especially those with a history of medication overuse. Patients typically take a series of classes where they learn relaxation methods, guided meditations, controlled breathing practices, and stress management.
Research and effectiveness
Many people with migraine tend to focus on the pain associated with the condition, which can lead to worsening outcomes. Thus, positive behaviors designed to reduce stress and relax both the mind and aspects of the body are generally steps forward in the treatment process. Research has generally supported that mindfulness and stress reduction techniques can be at least as effective as preventive medication, particularly for those previously diagnosed with medication overuse headache.15 In another study, meditation reduced pain by 33% for patients with chronic migraine after only a single session.16 Although other studies have not shown a significant reduction in the frequency of attacks, there is growing evidence that headache duration and disability can be improved as well as decreased stress and blood pressure observed in patients who practice these relaxation methods.17-18
Side effects
No reported side effects have been observed in mindfulness-based relaxation or stress reduction.
Cost
Like other migraine remedies, the cost of these treatments can vary greatly—from just a few dollars per session to $250—and often require multiple sessions. Self-guided meditation or related behavioral therapies can be a more cost-effective alternative. Our own Kerrie Smyres, a prominent patient advocate in the migraine community, recommends the book You Are Not Your Pain by Vidyamala Burch for the self-directed approach.
5. Yoga

The practice of yoga has been used for its therapeutic value for thousands of years, but it has enjoyed growing popularity since the 1970s. It is closely linked to relaxation and meditation, and accomplishes similar goals through movement and breathing techniques. Patients practicing yoga move through various stretches and hold specific poses while concentrating on deep breathing.
Research and effectiveness
The cumulative effect of yoga over time has shown to be a worthwhile source of alleviation for people with migraine, according to research. One analysis showed that patients who participated in 30 sessions of yoga over six weeks experienced a reduction in migraine frequency and intensity, particularly when coupled with more standard treatments.19 Another study revealed that not only did the number and intensity of migraine attacks go down, but overall pain levels, medication use, as well as anxiety and depression scores also decreased for those engaging in ongoing yoga therapy.20 Although the research has been positive, however, it should be noted that there are not many studies highlighting yoga as potential migraine therapy.
Side effects
As with most forms of exercise, the usual side effects of soreness, muscle tightness and joint pain can all occur with yoga. It’s always important to consult with a doctor to make sure you are capable of any type of physical exercise.
Cost
A private yoga session is not necessarily cheap, costing $60 per session on average, but it may be preferred in order to focus on specific pain points for migraine patients. Therapeutic yoga may be similarly expensive. And, as with other alternative forms of migraine treatment, it is likely that you will have to participate in multiple sessions in order to experience the full effect—this can make the cost of private yoga in the hundreds or thousands of dollars. However, group sessions may be a less expensive alternative. Look for yoga classes at your local gym for the cost of the membership, which could range anywhere between $10 to $50 per month.
6. Neurostimulation (Cefaly or Spring TMS)

While this might sound like an invasive surgical procedure, two non-invasive therapies broadly labeled “neurostimulation” or “neuromodulation” may offer relief for migraine. The first of these treatments, transcutaneous supraorbital nerve stimulation through a device called the Cefaly, uses electrodes to inhibit the onset of attacks in all types of migraine patients. The second, known as transcranial magnetic stimulation through the Spring TMS, utilizes magnets to stimulate cranial nerves and render the same effect.
Research and effectiveness
Approved by the Food & Drug Administration (FDA), transcutaneous supraorbital nerve stimulation with the Cefaly device has been directly examined in clinical research and was shown to be more effective than “sham” alternatives. In fact, studies have shown that it may reduce migraine attacks by as much as 50% per month, making it at least as viable as other drug and nondrug migraine prevention options.21 A small study also showed that it has the potential to break migraine attacks too, particularly those longer than 72 hours.22 The actual results cited by patients, however, may be less clear. In a clinical survey of people with migraine, just over half of all respondents reported satisfaction with Cefaly after using it for an average of nearly two months. The other half returned the device.23
Transcranial magnetic stimulation with the Spring TMS has also been approved by the FDA. Research has shown it to be particularly effective at the onset of attacks for those diagnosed with migraine with aura, bringing greater chance for easing pain at two hours than sham devices.24 Another study showed similar results in the overall reduction of pain for people with migraine.25 The evidence is less conclusive, however, for Spring TMS neurostimulation as a prophylactic treatment for chronic migraine when compared with placebo and other common migraine alternatives such as Botox.26-27 Ultimately, researchers agree that more studies are needed to better understand the impact of neurostimulation for people looking to naturally minimize pain and curb their migraine attacks.
Side effects
A very small percentage of users reported minor side effects related to the Cefaly or Spring TMS. These issues included:
- localized pain or inflammation
- fatigue
- insomnia
- headache immediately after use
Cost
Both of these therapies require a doctor's prescription, and you should check with your insurance company to see whether they will cover or reimburse the cost. Spring TMS is currently rentable for three months at $250 per month or for an entire year at $175 per month. Some customers may also qualify for discounts. The Cefaly device starts at $499 with additional reusable electrodes available for $25 to $33 per package. A copy of the medical prescription must be emailed or faxed to the company after placing an order.
7. Supplements (magnesium, riboflavin)

Supplements like magnesium and riboflavin are readily available as pills, and offer a natural solution for alleviating the pain of migraines. A possible reason for their effectiveness is due to observations that patients with the headache disorder may already have magnesium deficiency and lower levels in their brain during attacks. Similarly, riboflavin (also known as vitamin B2) deficiency may also exist.28-29 However, it is important to be aware of the potential side effects outlined for these migraine supplements.
Research and effectiveness
Like many migraine remedies, it can be difficult to draw clear conclusions about their effectiveness. What we do know is that high-dose riboflavin (200-400mg) was concluded in one study to have statistically significant effects on migraine frequency for adults—including a 50% reduction in attacks.30 The evidence is muddier as to whether or not riboflavin can act as a migraine preventative for children.31-32 And dosage may be an important factor as another study highlighted that lower doses (50mg) were no more viable than placebo pills.33 Similarly, higher amounts of magnesium have also shown promise in research, outperforming placebo in averting migraine attacks in at least two clinical studies; severity of attacks and other medication use were also lower in those taking high-dose magnesium for migraines.34-35 More data is needed, but certain researchers have acknowledged that it may be a more realistic option (and thus more effective) for migraine patients who have a known magnesium deficiency.36
Side effects
Several side effects have been reported with the use of magnesium and riboflavin for migraines, although the numbers have been small. These have included diarrhea, vomiting, and intestinal irritation. It is unclear if these side effects are directly related to the use of these specific migraine supplements, and there may be additional issues—such as difficulty breathing and muscle weakness—not identified in research but which occur in patients who take them. More information is needed, and it is always best to speak with your doctor about over-the-counter supplements.
Cost
Over-the-counter magnesium and riboflavin for migraine can typically cost between $5 to $50, depending on brand.
Conclusion
It can be hard finding researched-backed products and treatments that naturally provide relief for migraines without having to rely on prescription medications. That is why you will not see daith piercing on this list—which is a higly-debated "remedy" that simply does not have the evidence to support it as an effective therapy, especially when combined with patient stories of its often painful side effects. But you have to remember, each person responds differently to any given treatment, so talk with your doctor or headache specialist about each of these options to see what might be best for you.
References:
1 Plank S, Goodard JL, Pasierb L, Simunich TJ, Croner JR. Standardized set-point acupuncture for migraines. Altern Ther Health Med. 2013 Nov-Dec;19(6):32-7.
2 Jena S, Witt CM, Brinkhaus B, Wegscheider K, Willich SN. Acupuncture in patients with headache. Cephalalgia. 2008 Sep; 28(9):969-79.
3 Linde K, Allais G, Brinkhaus B, Manheimer E, Vickers A, White AR. Acupuncture for migraine prophylaxis. Cochrane database of systematic reviews (Online). 2009;(1):CD001218. doi:10.1002/14651858.CD001218.pub2.
4 Wonderling D, Vickers AJ, Grieve R, McCarney R. Cost effectiveness analysis of a randomised trial of acupuncture for chronic headache in primary care. BMJ : British Medical Journal. 2004;328(7442):747. doi:10.1136/bmj.38033.896505.EB.
5 Stokes DA, Lappin MS. Neurofeedback and biofeedback with 37 migraineurs: a clinical outcome study. Behavioral and Brain Functions : BBF. 2010;6:9. doi:10.1186/1744-9081-6-9.
6 Mullally WJ, Hall K, Goldstein R. Efficacy of biofeedback in the treatment of migraine and tension type headaches. Pain Physician. 2009 Nov-Dec;12(6):1005-11.
7 Nestoriuc Y, Martin A. Efficacy of biofeedback for migraine: a meta-analysis. 2007. In: Database of Abstracts of Reviews of Effects (DARE): Quality-assessed Reviews [Internet]. York (UK): Centre for Reviews and Dissemination (UK); 1995-.
8 Hammond D.C. Kirk L. Negative Effects and the Need for Standards of Practice in Neurofeedback. Biofeedback. Volume 35, Issue 4, pp. 139–145.
9 M. Tatsumoto, T. Eda, T. Ishikawa, M. Ayama, K. Hirata “Light of Intrinsically Photosensitive Retinal Ganglion Cell (ipRGC) Causing Migraine Headache Exacerbation.” IHC symposium OR3. 2013 June.
10 Good, P.A., Taylor, R.H. and Mortimer, M.J. (1991), The Use of Tinted Glasses in Childhood Migraine. Headache: The Journal of Head and Face Pain; 31: 533–536. doi:10.1111/j.1526-4610.1991.hed3108533.x
11 Wilkins, A. J. and Wilkinson, P. (1991), A tint to reduce eye-strain from fluorescent lighting? Preliminary observations. Ophthalmic and Physiological Optics, 11: 172–175. doi:10.1111/j.1475-
12 Blackburn MK, Lamb RD, Digre KB, et al. FL-41 Tint Improves Blink Frequency, Light Sensitivity, and Functional Limitations in Patients with Benign Essential Blepharospasm. Ophthalmology. 2009;116(5):997-1001. doi:10.1016/j.ophtha.2008.12.031.
13 Clark J, Hasselfeld K, Bigsby K, Divine J. Colored Glasses to Mitigate Photophobia Symptoms Posttraumatic Brain Injury. J Athl Train. 2017 Aug;52(8):725-729. doi: 10.4085/1062-6050-52.4.04. Epub 2017 Jun 26.
14 Wilkins AJ, Baker A, Amin D, Smith S, Bradford J, Zaiwalla Z, Besag FM, Binnie CD, Fish D. Treatment of photosensitive epilepsy using coloured glasses. Seizure. 1999 Dec;8(8):444-9.
15 Grazzi L, Sansone E, Raggi A, et al. Mindfulness and pharmacological prophylaxis after withdrawal from medication overuse in patients with Chronic Migraine: an effectiveness trial with a one-year follow-up. The Journal of Headache and Pain. 2017;18(1):15. doi:10.1186/s10194-017-0728-z.
16 Tonelli ME, Wachholtz AB. Meditation-Based Treatment Yielding Immediate Relief for Meditation-Naïve Migraineurs. Pain management nursing : official journal of the American Society of Pain Management Nurses. 2014;15(1):36-40. doi:10.1016/j.pmn.2012.04.002.
17 Wells, R. E., Burch, R., Paulsen, R. H., Wayne, P. M., Houle, T. T. and Loder, E. (2014), Meditation for Migraines: A Pilot Randomized Controlled Trial. Headache: The Journal of Head and Face Pain, 54: 1484–1495. doi:10.1111/head.12420.
18 Oberg EB, Rempe M, Bradley R. Self-directed Mindfulness Training and Improvement in Blood Pressure, Migraine Frequency, and Quality of Life. Global Advances in Health and Medicine. 2013;2(2):20-25. doi:10.7453/gahmj.2013.006.
19 Kisan R, Sujan M, Adoor M, et al. Effect of Yoga on migraine: A comprehensive study using clinical profile and cardiac autonomic functions. International Journal of Yoga. 2014;7(2):126-132. doi:10.4103/0973-6131.133891.
20 John, P.J., Sharma, N., Sharma, C. M. and Kankane, A. (2007), Effectiveness of Yoga Therapy in the Treatment of Migraine Without Aura: A Randomized Controlled Trial. Headache: The Journal of Head and Face Pain, 47: 654–661. doi:10.1111/j.1526-4610.2007.00789.x
21 Schoenen J, Vandersmissen B, Jeangette S, Herroelen L, Vandenheede M, Gérard P, Magis D. Migraine prevention with a supraorbital transcutaneous stimulator: a randomized controlled trial. Neurology. 2013 Feb 19;80(8):697-704. doi: 10.1212/WNL.0b013e3182825055. Epub 2013 Feb 6.
22 M Kozminski. Transcutaneous supraorbital nerve stimulation as a rescue therapy. American Headache Society 56th Annual Scientific Meeting. Los Angeles, CA. 2014.
23 Magis D, Sava S, d’ Elia TS, Baschi R, Schoenen J. Safety and patients’ satisfaction of transcutaneous Supraorbital NeuroStimulation (tSNS) with the Cefaly® device in headache treatment: a survey of 2,313 headache sufferers in the general population. The Journal of Headache and Pain. 2013;14(1):95. doi:10.1186/1129-2377-14-95.
24 Lipton RB, Dodick DW, Silberstein SD, Saper JR, Aurora SK, Pearlman SH, Fischell RE, Ruppel PL, Goadsby PJ. Single-pulse transcranial magnetic stimulation for acute treatment of migraine with aura: a randomised, double-blind, parallel-group, sham-controlled trial. Lancet Neurol. 2010 Apr;9(4):373-80. doi: 10.1016/S1474-4422(10)70054-5. Epub 2010 Mar 4.
25 Clarke BM, Upton ARM, Kamath MV, Al-Harbi T, Castellanos CM. Transcranial magnetic stimulation for migraine: clinical effects. The Journal of Headache and Pain. 2006;7(5):341-346. doi:10.1007/s10194-006-0329-8.
26 Schwedt TJ, Vargas B. Neurostimulation for Treatment of Migraine and Cluster Headache. Pain medicine (Malden, Mass). 2015;16(9):1827-1834. doi:10.1111/pme.12792.
27 Shehata HS, Esmail EH, Abdelalim A, et al. Repetitive transcranial magnetic stimulation versus botulinum toxin injection in chronic migraine prophylaxis: a pilot randomized trial. Journal of Pain Research. 2016;9:771-777. doi:10.2147/JPR.S116671.
28 Trauinger A, Pfund Z, Koszegi T, et al. Oral magnesium load test in patients with migraine. Headache. 2002;42: 114–119.
29 Mauskop A, Altura BM. Role of magnesium in the pathogenesis and treatment of migraine. Clin Neurosci. 1998; 5:24–27.
30 Boehnke, C., Reuter, U., Flach, U., Schuh-Hofer, S., Einhäupl, K. M. and Arnold, G. (2004), High-dose riboflavin treatment is efficacious in migraine prophylaxis: an open study in a tertiary care centre. European Journal of Neurology, 11: 475–477. doi:10.1111/j.1468-1331.2004.00813.x
31 Schoenen J, Jacquy J, Lenaerts M. Effectiveness of high-dose riboflavin in migraine prophylaxis. A randomized controlled trial. Neurology. 1998 Feb;50(2):466-70.
32 MacLennan SC, Wade FM, Forrest KM, Ratanayake PD, Fagan E, Antony J. High-dose riboflavin for migraine prophylaxis in children: a double-blind, randomized, placebo-controlled trial. J Child Neurol. 2008 Nov;23(11):1300-4. doi:10.1177/0883073808318053.
33 Bruijn J, Duivenvoorden H, Passchier J, Locher H, Dijkstra N, Arts WF. Medium-dose riboflavin as a prophylactic agent in children with migraine: a preliminary placebo-controlled, randomised, double-blind, cross-over trial. Cephalalgia. 2010 Dec;30(12):1426-34. doi: 10.1177/0333102410365106. Epub 2010 Mar 26.
34 Emel Köseoglu, Abdullah Talaslıoglu, Ali Saffet Gönül, Mustafa Kula . The effects of magnesium prophylaxis in migraine without aura. Magnesium Research. 2008;21(2):101-108. doi:10.1684/mrh.2008.0132.
35 Peikert A, Wilimzig C, Köhne-Volland R. Prophylaxis of migraine with oral magnesium: results from a prospective, multi-center, placebo-controlled and double-blind randomized study. Cephalalgia. 1996 Jun;16(4):257-63.
36 Mauskop A, Varughese J. Why all migraine patients should be treated with magnesium. J Neural Transm (Vienna). 2012 May;119(5):575-9. doi: 10.1007/s00702-012-0790-2. Epub 2012 Mar 18.

TheraSpecs® Glasses for Light Sensitivity
Find the glasses that fit your needs and lifestyle, and stay protected from screens, fluorescents, unwanted blue light, sunlight, flashing lights, and more.
Shop Now



