7 Possible Ways to Manage Photophobia (+ Other Relief Tips)
Photophobia, which refers to a strong and often painful sensitivity to light, can be frustrating for those who have it; the symptom can cause physical discomfort, trigger other symptoms, and negatively impact daily life. It is also not easily treated on account of the fact that there is no medication which is widely proven to reduce its effects, and you cannot just hide from all light either. But various options do exist for treating photophobia, and we curate remedies that are known to provide some relief.
Note: These likely do not reflect all of the potential therapies available to patients, but they have at least some effectiveness in relieving light-related pain according to documented clinical studies—many of which we cite below.

Precision-tinted glasses
The single-most effective tool for combating photophobia is precision-tinted glasses, specifically those tinted with FL-41. Research has shown these lenses to relieve even the most chronic of light-sensitive individuals, whether they have migraine, blepharospasm, post-concussion syndrome or another disorder. The reason they work centers on their filtering of light that can activate the eyes and the brain in such a way so as to cause pain and other symptoms.1
They even help reduce generalized light sensitivity, particularly from fluorescents, by cutting down on the invisible pulsing that conventional fluorescent lighting and even some digital screens emit.2 So even though they were designed for people with chronic light sensitivity, they can be just as—if not more—effective than so-called “blue blockers” for people who are only sensitive to artificial blue light.
Here are just some of the recorded benefits of these specialty glasses:3,4
- 74 percent reduction in attacks for people with migraine-related photophobia
- Improvement in overall light sensitivity, spasm frequency and severity for people with blepharospasm
- Greater long-term reduction of harmful, light-triggered brain activity
Although each of these studies represent a small sample size, thousands more have tried these precision-tinted glasses as a treatment for photophobia and experienced similar relief. While they have been most popular with migraine patients (such that the phrase ‘migraine glasses’ has become part of the lexicon), they have anecdotal support among people with numerous other conditions—everything from meniere’s disease to mal de debarquement syndrome. Hundreds of medical professionals also recommend them for their patients with traumatic brain injuries, chronic headache disorders and vestibular conditions too.

Thousands with light sensitivity have found relief with TheraSpecs precision-tinted glasses.
Better yet, these lenses allow more light in than traditional sunglasses, so they are not simply another mechanism for "avoiding" light; this also means there is no added risk for dark adaption and worsening of photophobia. And yes, even those who chronically wear sunglasses inside all the time can have success with the lighter FL-41 tinted glasses.
Botox injections
Most of us would probably associated Botox® (or botulinum toxin A) injections with cosmetic use, but they have practical benefits for neurologic-based photophobia. Specifically, studies have shown that these injections can be effective for people with migraine-related photophobia (particularly those with comorbid dry eye symptoms) and reduce light sensitivity associated with blepharospasm too.5,6 There is emerging evidence that Botox® may also be an alternative treatment for traumatic brain injuries, but more research is needed to make a conclusive determination.7
Of course, there can be some downsides to using Botox® for chronic photophobia, specifically due to the possibility of unpleasant side effects. Some have reported issues such as skin irritation and muscle weakness around the injection site, headache, neck stiffness, and blurry vision. In addition, it was not designed for treating light-sensitive disorders, so it is more of a ‘happy coincidence’ that it has any effectiveness at all. And so for these reasons, leading advocacy organizations often recommend trying other prevention methods first, especially for migraine.8
Anti-CGRP medications
One of the most exciting developments for people with chronic migraine has been the approval of specific medications that can treat and even prevent attacks—and which also can dramatically reduce photophobia. These drugs target a protein released in the brain called "calcitonin gene-related peptide" (CGRP) that has been linked to symptomatic pain during a migraine episode. Here is a shortlist of these new FDA-approved anti-CGRP medications:
- Fremanezumab (AjovyTM)
- Erenumab (AimovigTM)
- Galcanezumab (EmgalityTM)
So how effective are they for also lessening the onset of light sensitivity? Multiple studies have shown they not only lower the frequency of attacks, but they tone down photophobia and other sensory symptoms.9,10 In addition, they reduce the total number of "headache days" that also feature sensitivity to light.11 And these results may be sustained for twelve weeks or more.12 These encouraging outcomes reinforce the importance of developing targeted therapies for chronic conditions like migraine because they can yield some of the biggest improvements in related issues like photophobia.
Of course, as with other medications, there are side effects of which patients should be aware. Since CGRP inhibitors are typically applied through injections, skin irritation and pain can occur. In addition, elevated anxiety or depression, constipation and/or diarrhea have been noted as well.12 Lastly, each of these medications have subtle differences, so it is important to work with your doctor prior to starting or changing any treatment.
Triptans
Unlike anti-CGRP medications, tryptamine-based medications (triptans for short) have been around for several decades as a treatment for acute migraine—meaning they are designed to stop an attack after it has already begun. So while they are unlikely to prevent the light-sensitive reactions of patients over time, they have at least been shown to relieve them within the first few hours (if not sooner) of a migraine attack; they can have similarly positive outcomes for pediatric migraine patients as well.13-16 They also can lead to a faster recovery time and quicker return to daily activities, which is known to be one of the most challenging side effects for people with photophobia. And the earlier these medications can be taken after the onset of pain, the more effective they are likely to be.
Common complaints associated with the oral use of triptans include: dizziness, dry mouth, fatigue, abnormal skin sensations (tingling, warmth, etc.), and headache that is separate from the migraine pain. So they are not free of side effects.
Transcutaneous electrical nerve stimulation
It sounds kind of scary, but transcutaneous electrical nerve stimulation (TENS) is a form of neuromodulation that sends electrical currents to parts of the brain via the surface of the skin. This process mediates pain and sensory responses from the nervous system, and it can be a treatment for persistent photophobia because it attempts to counteract activation of the trigeminal nerve—which is believed to be one of the main pathways for light-related pain.
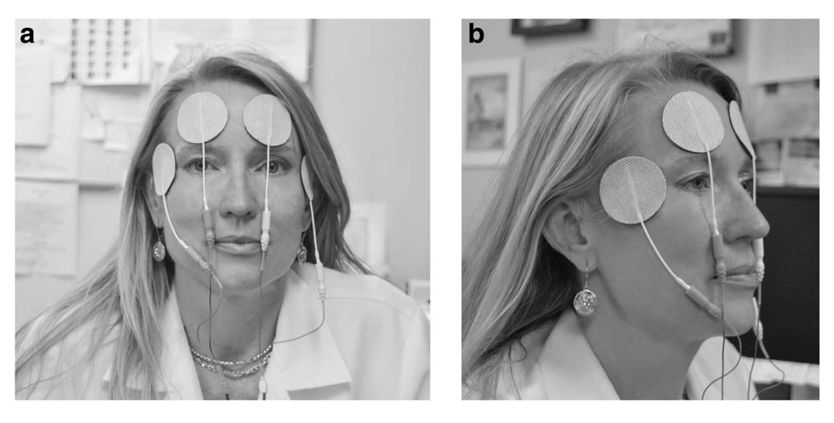
Woman using TENS unit for relief of ocular symptoms. Source: Neuromodulation Journal.
Unfortunately, only a few researchers have explored the benefits of this type of neuromodulation, but the results are promising. A small group of patients with dry eye had lower levels of photophobia in both eyes after the therapy and less overall pain; migraineurs may also experience fewer attacks, which of course can lead to a reduction in other symptoms like sensitivity to light as well.17,18 However, once again, this therapy can lead to unwanted side effects that cannot be overlooked.
Acetaminophen
Another temporary option for acute photophobia is the pain-relieving drug known as acetaminophen. Studies have suggested that these over-the-counter medications can alleviate some of the most burdensome migraine symptoms, especially light sensitivity, during the first two hours—which may last even longer for some.19 With greater accessibility and fewer adverse outcomes for most individuals, it can be a highly desirable therapy. But, as noted, it is unlikely to provide meaningful photophobia relief over the long haul and may not work at all for more chronic and/or medication-resistant disorders.
Pilocarpine
Pilocarpine is not a targeted treatment for light sensitivity, instead having been developed for people with chronic dry mouth and elevated inner-eye pressure (e.g. from Sjogren’s Syndrome). However, it has given some benefit to those with migraine-related photophobia. Immediate light sensitivity reduction was noted within an hour and sustained for at least one week for 70% of a small group of trial participants.20 It is important to note that—in addition to the known side effects of eye tearing, dizziness, and more—even medical experts advise that relief is only a short-term solution as light sensitivity symptoms typically return within 6 months.

Other tips for treating photophobia
Even though there is not a long list of relief therapies for light sensitivity, patients can make their dealings with light more comfortable with some additional tips and actions.
Pre-treatment
If you suspect you are sensitive to light, there are some important first steps you can take in order to address it. Here is what our team recommends:
Get a full work-up and diagnosis
Photophobia, particularly if it has come on all of a sudden, may signal a serious condition or injury. A comprehensive doctor’s visit will help identify the root cause of this sensitivity and help move forward with the appropriate treatment(s). Learn what causes photophobia ➜
Seek out specialists for the condition
While there are no medical professionals that focus solely on photophobia, there are countless specialists who treat the conditions that cause it. For instance, headache specialists are specifically educated to support those with migraine and its related symptoms. Find a headache specialist ➜
Specify the aggravating or triggering sources
Many photophobic patients can specify exact types of lighting that set off their episodes—from fluorescent lighting to LEDs to bright sunlight. Understanding these factors can lead to better long-term management. Test what triggers your photophobia ➜
Look out for emotional complications
Although light sensitivity is predominantly a physical reaction, emotional side effects can happen too. People with photophobia are known to have higher levels of anxiety and depression, both of which can make the physiological issues worse. This further reinforces the importance of a thorough exam. More about photophobia and anxiety ➜
Behavioral changes
Patients must not sacrifice long-term health for shorter term relief when it comes to dealing with photophobia. As we previously mentioned, the dark adaptation of the eyes is a real phenomenon that results from chronic light avoidance. Therefore, patients should abide by the following:
- Stop wearing sunglasses indoors regularly to prevent photophobic episodes
- Only use dark room or dim light environments during acute and/or extreme bouts of light sensitivity
- Find ways to manage light triggers instead of outright avoiding them
In fact, there are numerous ways to create a more light-friendly environment. This can include changes in the home, workplace accommodations and digital screen-related hacks. All of these can help make the lighting a little more tolerable so that you do not have to abandon your most cherished activities.
Other considerations
Patients must remember that photophobia often represents a complex and still-unknown process that may be further complicated by the specific disorder that is responsible for it. This can render even the most promising of treatments ineffective for any given person due to all the variables. We always recommend consulting with a physician or specialist to determine what works best for you.
That said, light-sensitive individuals can be encouraged by the fact that the symptom may simply decrease on its own over time. Although chronic photophobia is unlikely to fully remit as a person gets older, approximately half of TBI patients have reported a reduction in its effects over the years; migraine attacks (as well as their symptoms) may also become less frequent and intense after the age of fifty.21 Still, there is no cure for persistent sensitivity to light and many of the underlying conditions.
Lastly, there have been some exciting recent developments—specifically surrounding the role of green light therapy. Researchers found that only lighting on the green color spectrum might actually reduce brain hypersensitivity and corresponding pain, whereas all other colors have been shown to worsen migraine-related photophobia.22 However, follow-on studies have shown that it still negatively impacts attack symptoms in about 40% percent of migraineurs. In addition, any practical applications of green light for relief would have to account for the brightness levels because, after all, people with photophobia have a significantly lower tolerance for any light. Hopefully, we will see more exploration of this area in the future.
More resources:
Alternatives for Natural Migraine Relief and Prevention
8 Things to Avoid if You Have Light Sensitivity
Medications that May Increase Photophobia
Dark Adaptation: The Problem with Wearing Sunglasses Indoors
References:
1M. Tatsumoto, T. Eda, T. Ishikawa, M. Ayama, K. Hirata. Light of Intrinsically Photosensitive Retinal Ganglion Cell (ipRGC) Causing Migraine Headache Exacerbation. IHC symposium OR3. 2013 June.
2Wilkins AJ, Wilkinson P. A tint to reduce eye-strain from fluorescent lighting? Preliminary observations. Ophthalmic Physiol Opt. 1991 Apr;11(2):172-5.
3Good PA, Taylor RH, Mortimer MJ. The use of tinted glasses in childhood migraine. Headache. 1991 Sep;31(8):533-6.
4Blackburn MK, Lamb RD, Digre KB, et al. FL-41 tint improves blink frequency, light sensitivity, and functional limitations in patients with benign essential blepharospasm. Ophthalmology. 2009;116(5):997–1001. doi:10.1016/j.ophtha.2008.12.031
5Diel RJ, et al. Photophobia and sensations of dryness in patients with migraine occur independent of baseline tear volume and improve following botulinum toxin A injections. Br J Ophthalmol. 2018 Sep 29. pii: bjophthalmol-2018-312649. doi: 10.1136/bjophthalmol-2018-312649. [Epub ahead of print]
6Olson RM, Mokhtarzadeh A, McLoon LK, Harrison AR. Effects of Repeated Eyelid Injections with Botulinum Toxin A on Innervation of Treated Muscles in Patients with Blepharospasm. Curr Eye Res. 2019 Mar;44(3):257-263. doi: 10.1080/02713683.2018.1543707. Epub 2018 Nov 23.
7Yerry JA, Kuehn D, Finkel AG. Onabotulinum Toxin A for the treatment of headache in service members with a history of mild traumatic brain injury: a cohort study. Headache. 2015 Mar;55(3):395-406. doi: 10.1111/head.12495. Epub 2015 Feb 3.
8Bendtsen L, et al. Guideline on the use of onabotulinumtoxinA in chronic migraine: a consensus statement from the European Headache Federation. J Headache Pain. 2018 Sep 26;19(1):91. doi: 10.1186/s10194-018-0921-8.
9Bigal ME, Walter S, Rapoport AM. Fremanezumab as a preventive treatment for episodic and chronic migraine. Expert Rev Neurother. 2019 May 22:1-10. doi: 10.1080/14737175.2019.1614742. [Epub ahead of print]
10Dodick DW, Silberstein SD, Bigal ME, et al. Effect of Fremanezumab Compared With Placebo for Prevention of Episodic Migraine: A Randomized Clinical Trial. JAMA. 2018;319(19):1999–2008. doi:10.1001/jama.2018.4853
11Silberstein SD, Stauffer VL, Day KA, Lipsius S, Wilson MC. Galcanezumab in episodic migraine: subgroup analyses of efficacy by high versus low frequency of migraine headaches in phase 3 studies (EVOLVE-1 & EVOLVE-2). J Headache Pain. 2019 Jun 28;20(1):75. doi: 10.1186/s10194-019-1024-x.
12Raffaelli B, Mussetto V, Israel H, Neeb L, Reuter U. Erenumab and galcanezumab in chronic migraine prevention: effects after treatment termination. J Headache Pain. 2019 Jun 3;20(1):66. doi: 10.1186/s10194-019-1018-8.
13Cady RK, Dexter J, Sargent JD, et al. Efficacy of subcutaneous sumatriptan in repeated episodes of migraine. Neurology. 1993 Jul;43:1363-8.
14Derry CJ, Derry S, Moore RA. Sumatriptan (oral route of administration) for acute migraine attacks in adults. Cochrane Database Syst Rev. 2012;2012(2):CD008615. Published 2012 Feb 15. doi:10.1002/14651858.CD008615.pub2
15Klassen A, Elkind A, Asgharnejad M, Webster C, Laurenza A. Naratriptan is effective and well tolerated in the acute treatment of migraine. Results of a double-blind, placebo-controlled, parallel-group study. Naratriptan S2WA3001 Study Group. Headache. 1997 Nov-Dec;37(10):640-5.
16McKeage K. Zolmitriptan Nasal Spray: A Review in Acute Migraine in Pediatric Patients 12 Years of Age or Older. Paediatr Drugs. 2016 Feb;18(1):75-81. doi: 10.1007/s40272-015-0160-2.
17Sivanesan E, Levitt RC, Sarantopoulos CD, Patin D, Galor A. Noninvasive Electrical Stimulation for the Treatment of Chronic Ocular Pain and Photophobia. Neuromodulation. 2018 Dec;21(8):727-734. doi: 10.1111/ner.12742. Epub 2017 Dec 28.
18Tao H, Wang T, Dong X, Guo Q, Xu H, Wan Q. Effectiveness of transcutaneous electrical nerve stimulation for the treatment of migraine: a meta-analysis of randomized controlled trials. J Headache Pain. 2018;19(1):42. Published 2018 May 29. doi:10.1186/s10194-018-0868-9.
19Lipton RB, Baggish JS, Stewart WF, Codispoti JR, Fu M. Efficacy and Safety of Acetaminophen in the Treatment of Migraine: Results of a Randomized, Double-blind, Placebo-Controlled, Population-Based Study. Arch Intern Med. 2000;160(22):3486–3492. doi:10.1001/archinte.160.22.3486
20Motter B, Jackowski M. Photophobia and Light-Induced Headache: Novel Long-Term Effects of Pilocarpine. Invest. Ophthalmol. Vis. Sci. 2013;54(15):5333.
21Truong JQ, Ciuffreda KJ, Han MH, Suchoff IB. Photosensitivity in mild traumatic brain injury (mTBI): a retrospective analysis. Brain Inj. 2014;28(10):1283-7. doi: 10.3109/02699052.2014.915989. Epub 2014 Jun 19.
22Photophobia in migraine does not apply to green light, which may lessen headache severity. Nurs Stand. 2016 Jun 8;30(41):14-5. doi: 10.7748/ns.30.41.14.s17.

TheraSpecs® Glasses for Light Sensitivity
Find the glasses that fit your needs and lifestyle, and stay protected from screens, fluorescents, unwanted blue light, sunlight, flashing lights, and more.
Shop Now



